A recent study (Makary & Daniel, 2016) of medical errors have estimated preventable medical errors may account for as many as 251,000 deaths annually in the United States (U.S.).
They are also the third cause of death in the U.S. behind by cancer and cardiovascular disease. These errors result from breakdown in teamwork and communication primarily but there are also gaps at times in knowledge and technical skill. Innovative medical educational approaches are warranted to target all these areas and decrease this number. A valuable tool to assist with the safe delivery of health care and improvement in individual and team skills is medical simulation. This article presents an overview of the medical simulation capabilities of the Naval Medical Center Portsmouth and highlights its unique importance in the training of clinical personnel to bridge the transformation to a High Reliability Organization.
Introduction
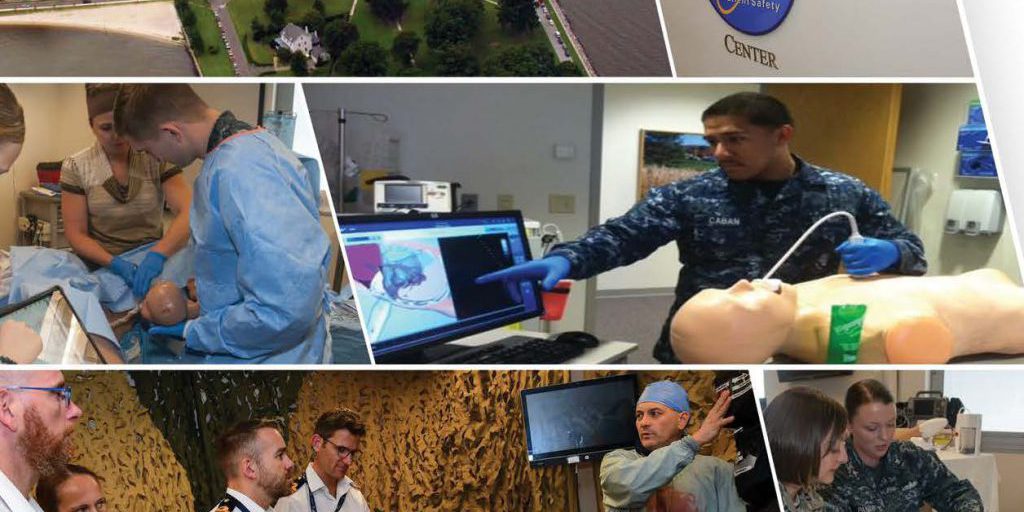
Naval Medical Center Portsmouth Healthcare Simulation and Bio-skills Training Center (NMCP HSBTC) has over 8,000 square feet of physical space and encompasses 5,720 square feet of contiguous space. It offers an immersive state of the art environment training room that accommodates a multitude of simulation related capabilities ranging from basic skills practice and training to large scale mass casualty scenario simulations. Simulation rooms for pediatrics, anesthesia, obstetrics, and virtual surgery are also available.
The simulation center maintains two multimedia related training conference rooms that have the ability to facilitate lecture, discussion, debriefs, webinars, and hands-on training. Staffing for the simulation center includes: NMCP HSBTC Director, Deputy Director, Manager, Nurse Educators, Simulation Technicians, and Research Scientist.
The simulation center is an integral part of 14 graduate medical education programs administered at NMCP. It provides weekly multi-disciplinary training sessions through the facilitation of safety and team-based trainings to all disciplines and specialties, and sustainment skills to hospital personnel. The center also provides immersive combat causality care training to deploying troops.
The simulation center was established in 2006 primarily to complement NMCP Graduate Medical Education programs. Over the past 12 years, the center has continued to strengthen the educational rigor of its curricular offerings. Specifically, it expanded into new and exciting areas of pre-deployment courses for military trauma surgical teams, and patient safety instructional programs that advance the teamwork and skill levels of the medical teams at NMCP. Importantly, during this period of growth, the simulation center was accredited by the American College of Surgeons in 2015.
NMCP HSBTC has provided simulation related training to over 26,000 Department of Defense (DoD) and civilian healthcare professionals since its inception. It has also expanded its simulation capabilities to over 50 different simulators. Simulation capabilities include: low and high-fidelity mannequins, task trainers, cut suits, standardized patients, and the latest in three-dimensional virtual simulation.
Targeted Training Curricula
The center has played an integral part in the development of several new simulation curricula: operational readiness for medical providers, corpsman and team-based simulation, nursing skill sustainment, and inter-professional team training evolutions such as the Perinatal Safety Stand-down.
In 2014, a seminal moment occurred when the Navy Specialty Leader for Interns requested that the simulation center develop a course for outgoing general medical officers that provided them with the opportunity, via a variety of medical simulators, to learn, rehearse, and be evaluated on their new core privileges prior to departure from NMCP. The end product of this tasker was the STOMP (Simulation Training for Operational Medicine Providers) curriculum, which has been administered at the simulation center for the past four years. Other DoD sites have also incorporated this curriculum into their training.
After the development and implementation of the STOMP curriculum, other areas developed similar skills curricula. Navy enlisted leadership developed a curriculum designed for corpsman who were transitioning back to the fleet. This simulation skills curricula are an integral part of the simulation center’s ongoing training and is titled HM FIRST (Corpsman Fleet Instructional Readiness and Simulation Training). The NESST (Nursing Enhanced Skills and Simulation Training) came to fruition through the efforts of the nursing staff to address nursing simulation needs for all newly arriving nurses and corpsman to the medical center. Internal medicine physicians also developed and implemented a simulation curriculum specific to their requirements necessary to maintain their core privileges in preparation for future deployments.
In addition, the center has facilitated multiple operational simulation courses, including Fleet Surgical Team pre-deployment training, Expeditionary Resuscitative Surgical System pre-deployment training, Role Two Light Maneuver, and Special Forces medic training. Table 1 presents an overview of the medical simulation training curricula at NMCP.
| Title | Overview | Audience |
| Operational Medical Providers (STOMP) | This provides an opportunity to rehearse and practice non-trauma primary care medicine skills in a proctored setting before practicing independently. | Physicians |
| Hospital Corpsman Fleet Instructional Readiness (HM FIRST) | This curriculum focuses on areas such as rapid assessment, physical examination, documentation, nail removal, wound closure, urinary catheterization and intravenous access. | Corpsman |
| Nursing Educational and Skills (NESST) | This simulation provides a proctored setting for the actual hands-on practice of day-to-day tasks that are expected of nurses who work the floors of the medical center. | Nurses and Corpsman |
| Fleet Surgical Teams | This program ensures Fleet Surgical Teams integrate with the crew of the amphibious assault ships (LHDs/LHAs) through rehearsal of trauma casualties using simulated patient and high-fidelity manikin exercises in preparation for primary Role 2 support activity during deployment. | Physicians, Nurses, and Corpsman |
| Expeditionary Surgical Resuscitative Surgical Systems (ESRSS) or Role Two Light Maneuver (R2LM) | This training is geared specifically for the smaller seven- to nine-person Damage Control Surgery Teams that may be called on to perform Role 2 capabilities on a wide range of diverse platforms at sea or ashore with team performance and resiliency goals similar to those of the Fleet Surgical Team Training. | Physicians, Nurses, and Corpsman |
Table 1. Overview of Medical Simulation Training Curricula at NMCP
Readiness through Research
Research-related efforts at the HSBTC focus on maximizing the readiness of our medical teams to promote patient safety and optimize quality health care delivered to operational forces and their families through simulation modalities.
NMCP simulation center research endeavors are all IRB approved and fall into the following categories: Operational/in-garrison care, MTF-based simulation research, and Combat & Casualty Care. Table 2 presents an overview of the NMCP research endeavors.
| Category | Overview |
| Operational/in-garrison care | Examine the effectiveness of simulation training to improve in-garrison care by corpsmen (HM First), General Medical Officers (STOMP), and Internal Medicine physicians (IM Sustain). |
| MTF-based simulation research | IRB-approved protocols investigating application-based training for crash cart familiarization, obstetric simulation training and teamwork (OB-STaT) to reduce postpartum hemorrhage, the simulated Electronic Fetal Monitoring app in conjunction with the University of Tennessee-Knoxville, and pediatric confidence and skill in managing high-risk, low-volume pediatric emergency scenarios. |
| Combat & Casualty Care | Collaborating with investigators from Old Dominion University on a protocol entitled “The Development of an Innovative Role 2 CPG-based Trauma Patient Knowledge-Assessment Instrument and Training Materials that utilize Deliberative Practice and Mastery Training.” This protocol is developing a game-based assessment of trauma knowledge for healthcare providers in Role 2 environments. A second collaborative project that will be initiated shortly with investigators from Purdue University will investigate the effectiveness of tele-mentoring in trauma surgeries and is entitled “See-What-I-Do: Increasing Mentor and Trainee Sense of Co-presence in Trauma Surgeries with the STAR platform. |
Table 2. NMCP Research Endeavors
Previous research efforts supported by the simulation center centered on improving tactical combat casualty care (TCCC) and included simulation training that investigated skill retention in the use of the ITClamp™ for junctional hemorrhage, training and communication for en-route care providers, device stability in simulated casualty movement, and the use of tension pneumothorax cadaver models to determine optimum location of needle decompression.
Future related research areas of interest include: the impact of noise on team performance in austere environments, junctional hemorrhage control with REBOA, bleeding control skills for non-medical personnel, and more TCCC-related issues.
Medical Simulation Mannequins
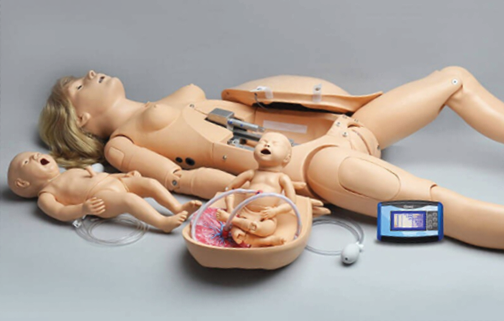
NOELLE® S550 Maternal and Neonatal teaching system
Medical simulation technology and the use of high-fidelity patient simulators are a key ingredient to the center’s immersive training curricula. The NMCP medical simulation center has a full array of these high-fidelity mannequins. For obstetric and birthing simulation, the simulation center employs the NOELLE® S550 Maternal and Neonatal teaching system (Gaumard, Inc.), permitting students to appreciate the complete birthing experience from the onset of labor, to delivery, along with treatment of the mother and neonate after delivery. It provides capabilities in ALS, obstetrics, and neonatal resuscitation protocols. Features of the system are presented in Table 3.
| NOELLE® S550 Maternal and Neonatal Teaching System Features | ||
| Full size articulating full-body female | Intubatable airway with chest rise | IV arm for meds/fluids |
| Removable stomach cover | Practice Leopold Maneuvers | Multiple fetal heart sounds |
| Automatic birthing system | Measures head descent and cervical dilation | Multiple placenta locations |
| Replaceable dilating cervices | Practice postpartum suturing on vulval inserts | One articulating birthing baby with placenta |
Table 3. NOELLE® S550 Maternal and Neonatal teaching system features
Another regularly used mannequin at the NMCP simulation center is the SimMan 3G (Laerdal, Inc.). This simulator is an advanced adult patient simulation system that facilitates training of basic and advanced life support, as well as allowing a full array of patient examination techniques and complex patient-care scenarios. The system allows the instructor to effectively assess the learner’s individual and teamwork skills in a realistic clinical scenario.
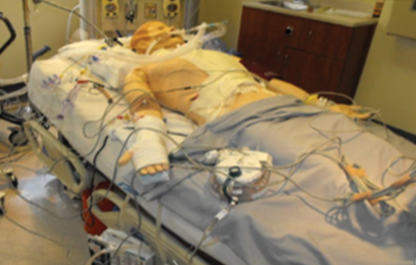
SimMan 3G Simulation System
SimMan 3G allows observation and recognition of most vital signs and invasive hemodynamic parameters. This can be achieved through clinical interaction with the mannequin, as well as observation of the mannequin’s homonymic status as viewed on the SimMan 3G Patient Monitor PC. Features of the SimMan 3G simulation system are presented in Table 4.
| SimMan 3G Simulation System Features | ||
| advanced configurable airway | Eyes that respond to light | Palpable Pulses |
| Lung, Heart, and Bowel Sounds | Convulsions simulate seizures or small hand movements | Bleeding and Wound Modules are fed from an internal blood reservoir |
| Vascular Access (intra-osseous) via the tibia and sternum | Auto-measurement of volume and concentration for drugs and IV fluids. | RFID Technology for automatic recognition of drugs and airway devices |
| Simulated Secretions: Sweat, tears, froth, urine and ear fluids are fed from an internal fluid reservoir. | ||
Table 4. SimMan 3G simulation system features
Training numbers
As the largest military healthcare simulation laboratory in the Hampton Roads, Virginia area, the NMCP Simulation Center has continued to expand its support to both internal medical center trainees as well as operational forces in the region. In 2017, the simulation center provided 28,316 prep hours and 11,883 man training hours for simulation activities to a total of 3,196 participants (2025 providers, 336 nurses, and 835 others). The training sessions continue to be ranked highly by learners in terms of 1) objectives/information, 2) support, 3) ability to problem solve, 4) feedback; and 5) fidelity with 2018 average scores of 4.68 on a 5-point validated simulation quality scale.
Conclusion
The NMCP Medical Simulation Center provides a safe and controlled environment to teach a wide variety of technical and non-technical skills to medical personnel and to assess individual and team performance. The NMCP HSBTC remains at the forefront of medical simulation training, providing medical education consistent with highest educational standards and ethical principles on a daily basis. As Military Medicine begins to embrace “high-reliability” principles, interactive simulation education and rehearsal will become key to reducing variance in a complex patient-delivery system ashore, afloat, and in forward-deployed environments.
References
- Makary MA, Daniel M. Medical error-the third leading cause of death in the US. BMJ 2016; 353:i2139. doi:10.1136/bmj.i2139.